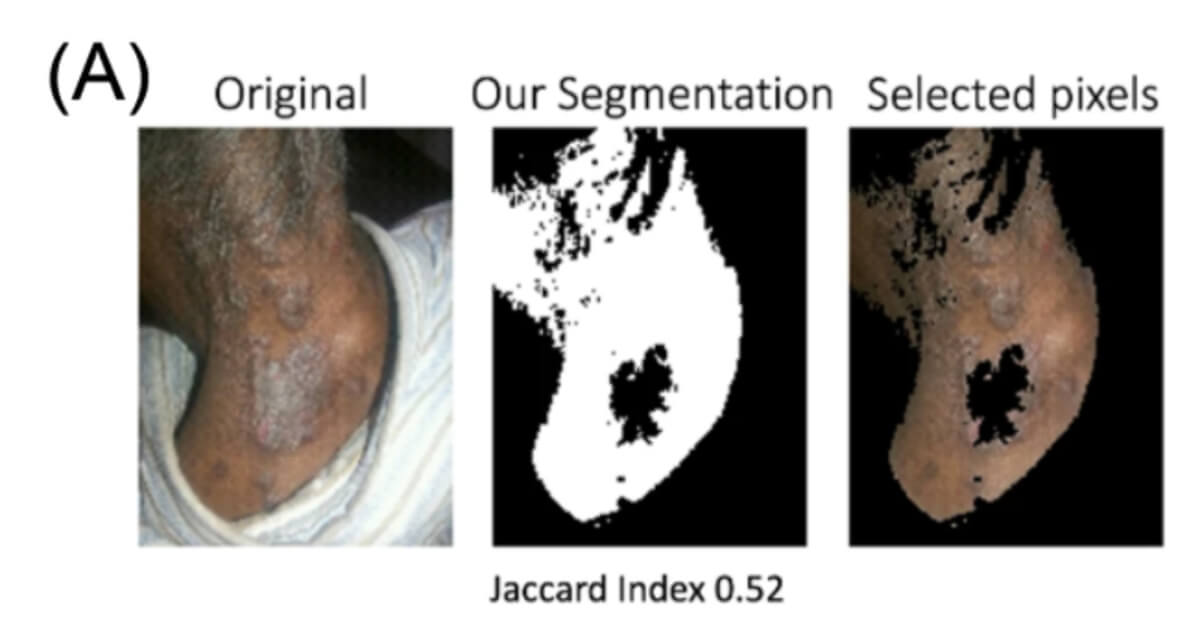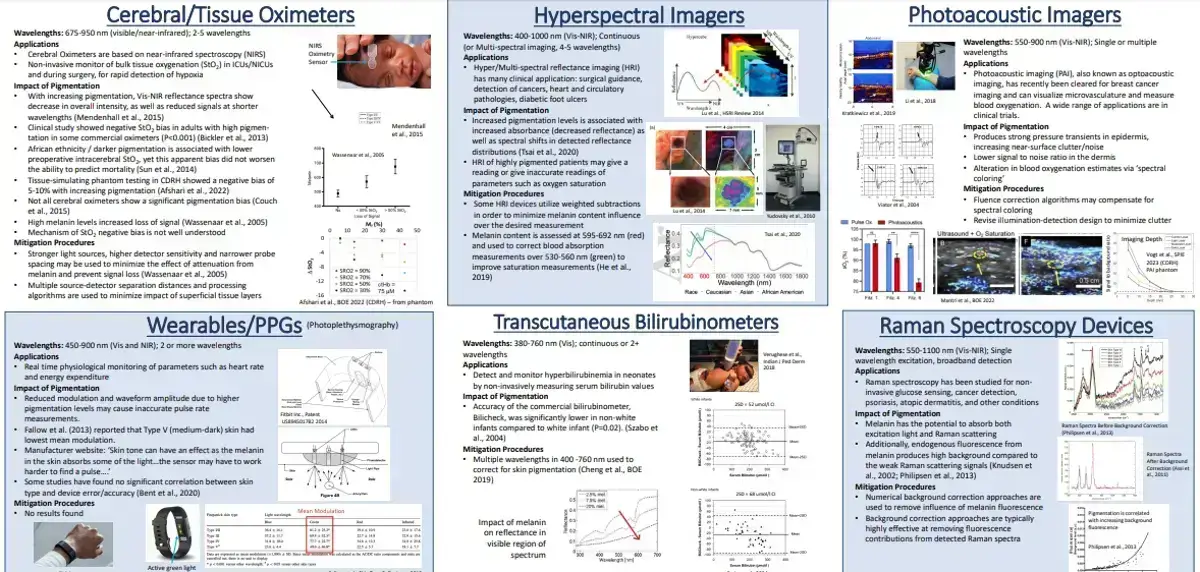
A recent 2023 study from the US FDA is titled “Impact of Skin Pigmentation on The Performance of Biomedical Optics Devices.” It is very interesting and the above poster image has very precise details spelled out. Make sure to also read my recent post on the lack of representation of darker skin in medical texts in the US and Western Europe.
Skin Pigment and Biomedical Device Performance
Melanin is recognized to be a major absorber of light in the skin. While melanin is the main factor in determining skin color, it can also significantly impact signals detected by optical medical devices. The authors of this latest study break out the biomedical devices analyzed into six categories:
- Cerebral/Tissue oximeters (675-950 nm wavelength).
- Hyperspectral imaging systems (400-1,000 nm).
- Photoacoustic imagers (550-900 nm).
- Wearables/PPGs (450-900 nm).
- Transcutaneous bilirubinometers (380-760 nm).
- Raman spectroscopy devices (550-1,100 nm).
In all six medical device types, the level of skin pigment in a patient makes a difference in how well each device works. What the authors call a skin pigmentation bias. The offer suggestions on mitigation procedure for all technologies other than for wearables/PPG (photoplethysmography).
Impact of Pigmentation and Solutions
Among the problems associated with increased skin pigment include:
- Reduced signals at shorter wavelengths.
- Intensity reduction.
- Reduced waveform modulation and amplitude.
- Excess device light absorption by the melanin in the skin.
- Undesired spectral shifts.
- Strong pressure transients in the epidermis, increasing near-surface clutter and noise.
- Lower signal to noise ratio in the dermis.
- Alteration in blood oxygenation estimates.
- Melanin has the potential to absorb both excitation light and Raman scattering.
Among the various mitigation measures that are suggested include: stronger light sources; higher detector sensitivity; narrower probe spacing; multiple source-detector separation distances and processing algorithms; weighted subtractions in hyperspectral reflectance imaging (HRI) devices; multiple wavelength utilization; fluence correction algorithms to compensate for spectral coloring; revision of illumination detection design; and numerical background correction approaches.
In recent years, clinical studies of pulse oximetry have garnered much attention in finding evidence of racial disparities in performance. This latest research indicates that other biomedical optics technologies can also be affected significantly by skin pigmentation levels in people of color.
Optical characteristics of skin melanin including absorption, scattering and fluorescence. There needs to be increased awareness by medical professionals in regards to the mechanisms and effects of epidermal melanin on detected optical signals. Feedback can help device manufacturers improve their technology. Moreover, government regulatory staff can then institute appropriate practices to avoid racial disparities in medical device efficacy.